Is there an egg in every follicle?
Unfortunately, not every follicle will yield an egg.
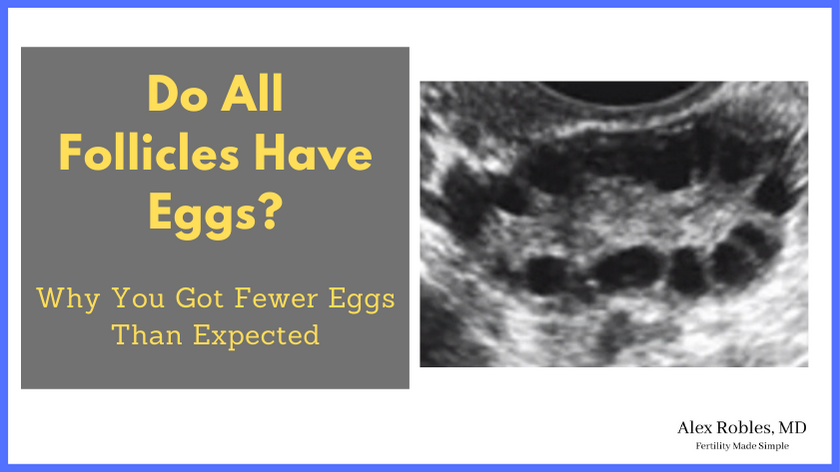
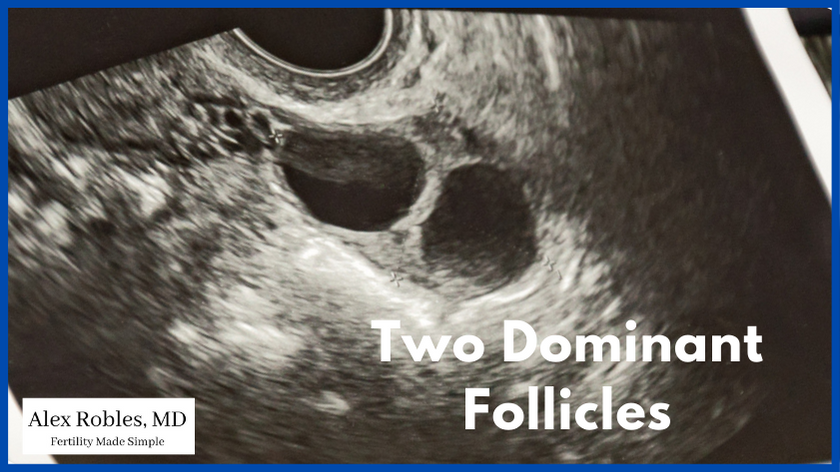
In a natural cycle, several antral follicles are recruited each month, but only one becomes dominant and gets released during ovulation. The others degenerate.
In an in vitro fertilization cycle, several follicles are allowed to grow and become dominant before they are retrieved.
In theory, each follicle contains an egg, but it is not uncommon for you to get fewer eggs than expected compared to the number of follicles you have.
How often is there no egg in a follicle?
Up to 20% or more of the follicles in an IVF treatment cycle do not yield an egg.
This number can be higher in women with polycystic ovarian syndrome (PCOS) with a high antral follicle count.
Why do some follicles not have eggs?
There can be many possible reasons why an egg is not retrieved from a follicle.
In general, the bigger the follicle, the more likely it is to yield an egg. Follicles that remain small throughout the stimulation are less likely to produce eggs.
Some women may also have empty follicle syndrome, a rare condition in which no eggs are retrieved following IVF stimulation.
One study found a correlation between empty follicles and diminished or low ovarian reserve (DOR).
In other words, the lower your reserve, the higher the chance of having empty follicles.
DOR can be detected by:
- low AMH levels (anti-mullerian hormone) (blood test)
- high FSH levels (blood test)
- low antral follicle count (seen on ultrasound scan)
Other researchers believe that empty follicles might be due to early oocyte atresia. This means that the egg cells degenerate as a result of abnormal or inadequate follicular growth.
With that said, there is some debate as to whether these follicles are truly empty.
So let’s cover some of the other reasons why eggs may not be collected.
Other reasons why some eggs are not collected
Some researchers believe that the follicles that don’t yield eggs do have eggs, but the egg does not detach from the follicular wall.
This could be due to incomplete follicular/oocyte maturity.
A second reason is premature ovulation.
Although rare, your follicles may rupture and release the egg before the egg retrieval. The risk of premature ovulation increases if your retrieval is delayed from when it is supposed to happen.
Lastly, there are other technical reasons why an egg may not be collected from a follicle.
Sometimes, a follicle can often be challenging to access. It can be very deep in the abdomen, next to a fibroid, or behind the uterus.
How do I know if my follicles contain eggs?
There is no way to determine if a follicle contains an egg until it is retrieved.
The diagnosis is always retrospective.
With that said, extremes of sizes usually indicate that the follicle is less likely to yield an egg.
Abnormally large follicles are frequently cysts, which by definition do not contain eggs.
In contrast, smaller follicles usually have not reached a big enough size to produce viable eggs. Even if an egg is retrieved from a small follicle, it is unlikely to be a mature egg.
What is the difference between mature eggs and immature eggs?
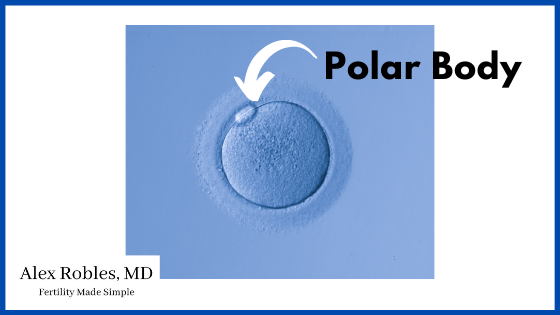
A mature egg has successfully divided its DNA in half and only contains 23 chromosomes instead of 46.
The other 23 chromosomes are extruded as a polar body.
An immature egg has not yet divided its DNA and still contains all 46 maternal chromosomes. As a result, immature eggs cannot be fertilized, as it needs to accept 23 chromosomes from the sperm.
What is the treatment for immature follicles?
Monitoring the size of your ovarian follicles through transvaginal ultrasound is the best way to predict if an egg will be mature.
Larger follicles are more likely to produce eggs that will reach full maturity.
If you had a low proportion of mature eggs in a previous cycle, your doctor might decide to let your follicles grow a little bigger the next time. Also, using a different type of trigger shot may help increase the eggs’ final maturation.
I discuss follicles in a lot more detail in this post.
Are eggs always stored in follicles?
All of your eggs are stored in structures called primordial follicles. Your eggs reside in these structures until they are recruited.
During a normal menstrual cycle, several of these primordial follicles develop into antral follicles. Usually, only one dominant follicle is allowed to continue its growth and gets released during ovulation.
The other antral follicles regress and degenerate.
The number of antral follicles you have at the beginning of a menstrual cycle correlates with your ovarian reserve and the number of potential eggs that would be available for retrieval.
How many follicles are normal in each ovary?
If you are under 35 years of age, approximately 6-10 antral follicles per ovary are within the expected range of normal ovarian reserve.
In contrast, if you have polycystic ovarian syndrome (PCOS), you may have 20 or more antral follicles in an ovary.
Also, keep in mind that your egg reserve is different from egg quality. You can have low reserve but good quality eggs and vice versa.
Unfortunately, we do not have a great way of measuring egg quality at this time.
Other Related Questions
What is a normal rate of follicle growth during IVF treatment?
Follicles usually grow 1-3 mm per day in a standard ovarian stimulation cycle.
Here is an example of a typical growth chart.
Follicle Growth Chart
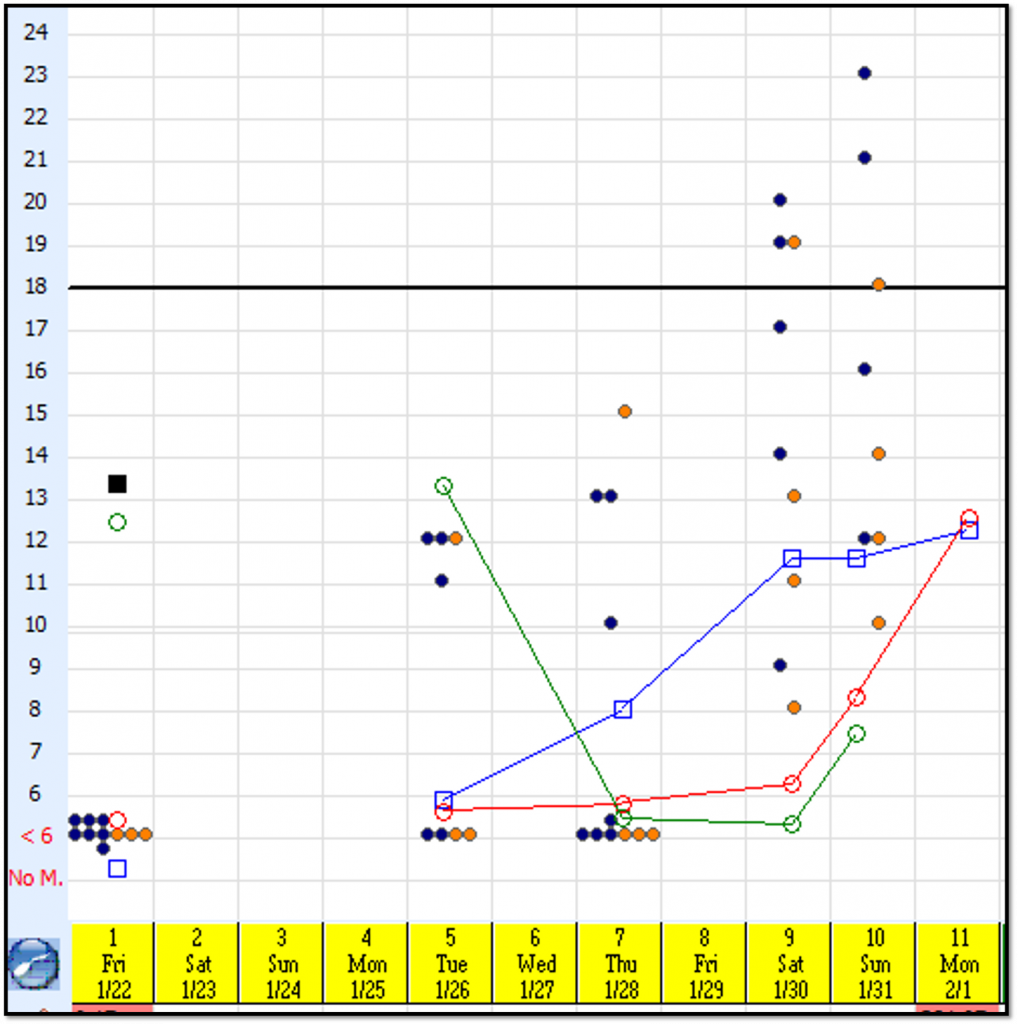
The x-axis is days of stimulation
The y-axis is size of follicle in millimeters
Each blue dot represents one follicle on the right ovary
Each orange dot represents one follicle on the left ovary
Can I get pregnant with a 16 mm follicle?
While getting pregnant with a 16mm follicle is possible, you also need to consider sperm quality, embryo competence, and uterine receptivity.
If the 16 mm follicle produces a mature egg, the egg then has to get fertilized.
After fertilization, the embryo has to grow and divide until it reaches the blastocyst stage.
At this point, the embryo will then need to implant into the uterine lining.
What is the minimum egg size needed to get pregnant?
In general, a 16-22 mm follicle is most likely to yield a mature egg, which is necessary for fertilization and pregnancy.
With that said, the egg is only one component necessary to achieve a healthy and successful pregnancy.
Other essential factors include sperm quality and uterine receptiveness.
Conclusion
Unfortunately, it is not possible to tell in advance which follicles will be empty and which will have eggs during an IVF cycle.
The only way to assess egg yield is after the egg retrieval procedure is already performed. Having had empty follicles doesn’t always mean a subsequent cycle will yield the same result.
Be sure to speak with your fertility doctor to learn what your options are.
Make An Appointment With Dr. Robles To Discuss Your Fertility Options Today!

Alex Robles, MD
Dr. Alex Robles is a Spanish-speaking Latino-American Reproductive Endocrinologist and Infertility specialist in New York City, and a board-certified OBGYN. He has a special interest in health, lifestyle, & nutrition. Make an appointment with Dr. Robles to discuss your fertility options today!
References:
- Madani T, Jahangiri N. Empty Follicle Syndrome: The Possible Cause of Occurrence. Oman Med J. 2015;30(6):417-420. doi:10.5001/omj.2015.83
- Revelli A, Carosso A, Grassi G, Gennarelli G, Canosa S, Benedetto C. Empty follicle syndrome revisited: definition, incidence, aetiology, early diagnosis and treatment. Reprod Biomed Online. 2017 Aug;35(2):132-138. doi: 10.1016/j.rbmo.2017.04.012. Epub 2017 May 23. PMID: 28596003.
- Abbara A, Vuong LN, Ho VNA, et al. Follicle Size on Day of Trigger Most Likely to Yield a Mature Oocyte. Front Endocrinol (Lausanne). 2018;9:193. Published 2018 Apr 25. doi:10.3389/fendo.2018.00193
