Are you starting an estrogen priming protocol before an in vitro fertilization cycle?
Do you want to know why we do it?
This article will provide an overview of
- what is estrogen priming,
- situations in which it can improve the ovarian response to IVF stimulation,
- and what IVF treatment protocols benefit from priming.
Let’s get started.

What Is Estrogen Priming?
Estrogen priming is the process of using estrogen pills in the preceding cycle before your IVF cycle to prepare your ovaries for stimulation.
The hope is that estrogen priming helps you respond better to IVF stimulation and have a more successful cycle.
What Does It Do?
Estrogen priming may enhance IVF stimulation by synchronizing the growth of your follicles.
You see, the goal of an IVF cycle is to grow multiple follicles so that we can collect as many eggs as possible during the egg retrieval procedure.
However, not every follicle grows at the same rate.
In addition, it is possible for you to have a larger follicle already growing before the stimulation phase begins.
In theory, priming the ovaries with estrogen may help prevent uneven growth of your follicles.
Estrogen priming can also be beneficial for patients who had a poor response in a previous IVF cycle.
More on that later.
Why Does Synchronized Growth Matter?
The benefit of having your follicles grow at similar rates is that it can increase the chance of obtaining the highest number of mature oocytes (eggs).
The bigger the follicle (~16-22 mm), the more likely we will retrieve a mature egg from it.
In contrast, smaller follicles (<14 mm) are more likely to yield no egg, or an immature egg.
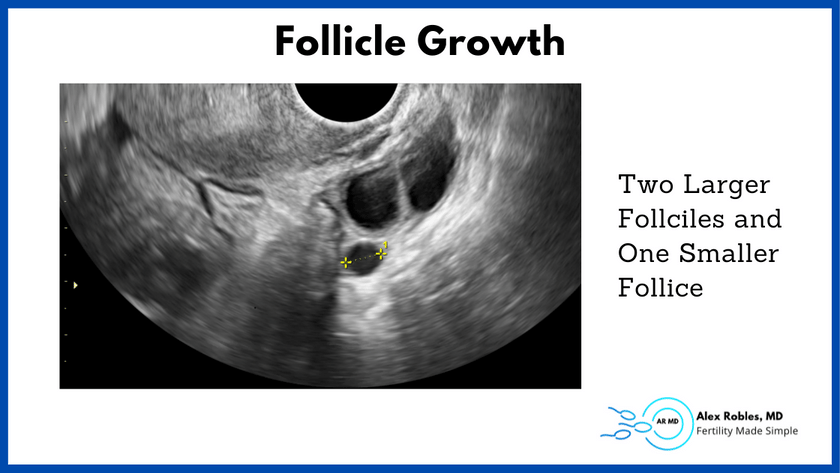
In an ideal world, all of your follicles would reach 16-22 mm at the same time, rather than having one or two follicles leading the others by a large margin.
There is only so much time you can give the smaller follicles to catch up once you have two or more follicles above 18 mm.
How Many Days Do You Need Estrogen Priming For?
Estrogen priming is typically done for about seven days before the start of controlled ovarian stimulation (the IVF cycle).
Before starting the pills, we need to wait until you are in the correct stage of your menstrual cycle (the luteal phase).
Some reproductive endocrinologists prefer to see you in the office to do an ultrasound and bloodwork first. This appointment ensures that you have ovulated and are in the luteal phase.
Other doctors feel comfortable having you start the medication seven days before your anticipated menstrual cycle.
One last option is using ovulation predictor kits.
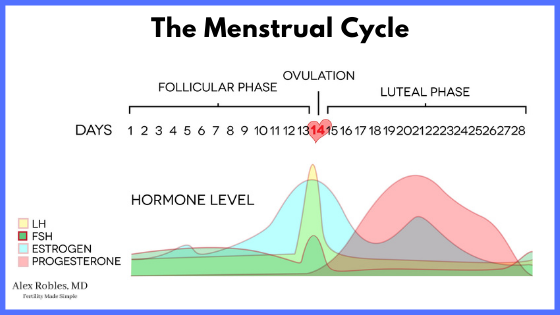
How To Use An Ovulation Predictor Kits To Time Luteal Phase Priming
An ovulation predictor kit (OPK) is another helpful tool to help you time your estrogen priming.
The OPK measures the luteinizing hormone (LH) in your urine, which will surge ~24 hours before you ovulate.
Start testing the OPK ~10 days after the start of your menstrual cycle. Most women will have a positive test on days 12-14. Once you get a positive test, wait exactly one week to ensure you are in the late luteal phase.
After the week, begin the estrogen pills until you get your next bleed.
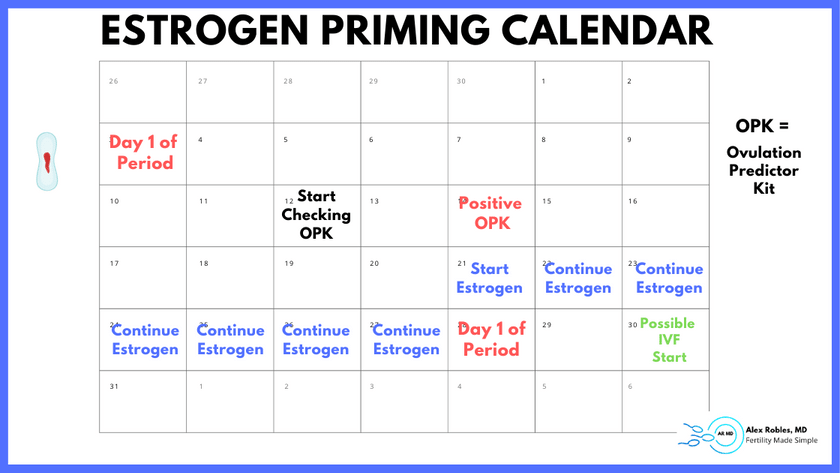
Estrogen Priming Protocol Calendar
Here is an example of the calendar for an estrogen priming protocol.
- Day 1: First day of your menstrual cycle
- Day 12: Positive ovulation predictor kit
- Day 20: Start estrogen priming
- Day 28 / Day 1: First day of your menstrual cycle – stop estrogen
- Day 3: Possible IVF start
What Is The Dose?
The recommended dose of estrogen for priming is 2 mg twice a day. You could also use an estrogen patch to get the same effect.
*Note: Estrogen priming is not the same as birth control pills.
Possible Side Effects of Estrogen Priming
The most common side effects of estrogen medication include
- headaches,
- bloating,
- nausea,
- mood changes
However, these side effects are usually mild and will dissipate after a few days.
Most patients don’t experience any side effects at all.
Does Estrogen Priming Help Egg Quality?
Unfortunately, estrogen priming does not improve egg or embryo quality.
As far as we know, there are no concrete strategies to improve egg quality.
The best thing that you can do is to live a healthy lifestyle which includes:
- eating a well-balanced diet,
- exercising regularly,
- avoiding smoking and other drugs,
- and managing stress.
Does It Reduce Antral Follicle Count?
Estrogen priming does not reduce the number of antral follicles you have at the start of an IVF cycle.
It does, however, prevent follicles from growing. This is how it works to synchronize follicular growth during controlled ovarian stimulation.
Is Priming Helpful For Poor Responders?
Estrogen priming may also be helpful for patients who have had a poor response to IVF treatment (aka, a poor responder).
Poor responders often have diminished ovarian reserve (DOR) and elevated levels of follicle-stimulating hormone (FSH).
This is problematic because FSH is the primary hormone we use to stimulate your ovarian follicles.
If your ovaries are already exposed to high levels of follicle-stimulating hormone, they are much less likely to respond to additional FSH injections.
In these cases, estrogen priming may improve ovarian responsiveness to the medications by reducing the levels of FSH in the body before the stim.
What Does The Data Say?
The data looks promising, but the clinical trials are not recent.
For example, a 2012 retrospective study of 155 poor responders found that patients who received luteal estradiol had a lower cycle cancellation rate and a higher number of oocytes at the egg retrieval than the control group. There was also a trend toward better fertilization rates, but those data did not reach statistical significance.
Other smaller studies had similar findings.
Does it Help Improve Clinical Pregnancy Rates?
Based on the available literature, estrogen priming may improve clinical pregnancy rates in poor responders.
A systematic review and meta-analysis of eight studies found that estrogen priming improved clinical pregnancy rates by 33%.
However, this study is from 2013 and has a relatively small sample size. More research is needed.
Does Priming Help Most With Specific Ovarian Stimulation Protocols?
We can use estrogen priming with any ovarian stimulation protocol. The most common IVF protocols include
- GnRH (gonadotropin releasing hormone) antagonist protocol: The GnRH antagonist protocol uses specific drugs to suppress the body’s production of FSH and LH to prevent premature ovulation.
- Microdose Flare protocol: This protocol uses the GnRH agonist Leuprolide (Lupron) as one of the primary drugs in the stimulation.
- Clomiphene citrate or letrozole protocols: These are milder forms of stimulation that can be used for low responders.
Conclusion
Luteal phase estradiol can be a useful tool for improving the follicular response in an ovarian stimulation cycle. Studies show that it can help synchronize follicular growth and reduce FSH levels in low responders.
However, more research is needed to determine if it can improve the clinical pregnancy or live birth rate.
Be sure to talk to your fertility doctor to learn if estrogen priming is right for you.
- The Oocyte Retrieval: What To Expect
- What Is A Good Number of Follicles For IVF?
- Did You Get A Lower Number of Eggs Then Expected? Here’s Why
Make An Appointment With Dr. Robles To Discuss Your Fertility Options Today!

Alex Robles, MD
Dr. Alex Robles is a Spanish-speaking Latino-American Reproductive Endocrinologist and Infertility specialist in New York City, and a board-certified OBGYN. He has a special interest in health, lifestyle, & nutrition. Make an appointment with Dr. Robles to discuss your fertility options today!
References:
- Chang EM, Han JE, Won HJ, Kim YS, Yoon TK, Lee WS. Effect of estrogen priming through luteal phase and stimulation phase in poor responders in in-vitro fertilization. J Assist Reprod Genet. 2012 Mar;29(3):225-30. doi: 10.1007/s10815-011-9685-7. Epub 2011 Dec 8. PMID: 22160464; PMCID: PMC3288134.
- Reynolds KA, Omurtag KR, Jimenez PT, Rhee JS, Tuuli MG, Jungheim ES. Cycle cancellation and pregnancy after luteal estradiol priming in women defined as poor responders: a systematic review and meta-analysis. Hum Reprod. 2013 Nov;28(11):2981-9. doi: 10.1093/humrep/det306. Epub 2013 Jul 25. PMID: 23887073; PMCID: PMC3795468.
