You had an embryo transfer and did not get pregnant.
What’s next?
The period after a failed IVF cycle is a difficult time for many people.
This article will give you helpful information on what to expect after a failed embryo transfer and how how to stay on track with your fertility treatments going forward.

Do you get your period if the embryo transfer fails?
There are two ways to know if your embryo transfer has failed.
- You have a negative pregnancy test ~9-10 days after the embryo transfer
- You get your period shortly after the pregnancy test
When should I expect my period after a failed IVF cycle?
If your embryo transfer has failed, you will get a period around the time that you would normally expect it.
The period will come approximately 10-12 days after a blastocyst transfer or 12-15 days after a cleavage embryo (Day 3 embryo) transfer.
Do you have a normal period after a failed transfer?
Your period may be heavier than usual, especially if you took medications to thicken your endometrial lining.
Whenever you get a period, the bleeding is from the shedding of the endometrial lining. The thicker the lining, the heavier the period.
In addition, this period might be a bit more painful than a regular period as more tissue is being shed.
It should, however, be similar in consistency to your average period.
Does IVF change your menstrual cycle?
The period after a failed IVF cycle is similar to your regular menstrual cycle. However, it may be more painful and heavy.
Endometrial thickening medications will increase the amount of tissue that you will shed during this time.
After that time, your menstrual cycle should return to normal.
What actually happens when IVF implantation fails?
Implantation is when the embryo attaches to the lining of your uterus.
In a failed implantation, the embryo did not successfully attach to the endometrial lining.
A failed implantation could mean one of two things. There could be a problem with embryo quality, or endometrial receptivity could be an issue.
Why do some embryos not implant?
There are many possible reasons why an embryo doesn’t implant.
If you were able to make a blastocyst embryo, two main things could affect embryo implantation
- There is some inherent issue with the embryo
- The uterus isn’t prepared for implantation
Let’s go over both of these in more detail.
Embryo Assessment
At this time, there are only three ways to assess embryo quality.
- Embryo morphology
- Timing of blastulation
- Ploidy status as determined by pre-implantation genetic testing (PGT aka PGS)
Embryo morphology refers to the physical appearance of the embryo. Each embryo receives a grade based on how much it has expanded and how organized the cells are.
In theory, the better the morphology, the better the chance for a successful pregnancy.
The timing of blastulation refers to when the embryo reached the blastocyst stage.
Embryos should reach the blastocyst stage on days 5, 6, or 7. The earlier it makes it to blast, the greater the chance for success.
Lastly, ploidy status is determined by pre-implantation genetic testing, which is an embryo biopsy.
This test checks the number of chromosomes in each embryo and determines if there are any chromosomal abnormalities or missing or extra chromosomes.
Even with PGT, there may be some other underlying genetic defects not associated with chromosome numbers.
Aside from that, there aren’t any other reliable ways to assess the quality of the embryo.
Uterine Lining Assessment
There are a few ways to assess the quality of the endometrial lining.
The most common method is an ultrasound measurement of uterine thickness. Lining thickness has been shown to correlate with implantation, though this is only an indirect way to determine uterine receptivity.
There is also a test called the endometrial receptivity assay (ERA) for short.
This test aims to better determine uterine receptivity by looking at the gene expression level of an endometrial biopsy.
In other words, we are looking to see if your uterine lining is “receptive” at the time that an embryo would be transferred.
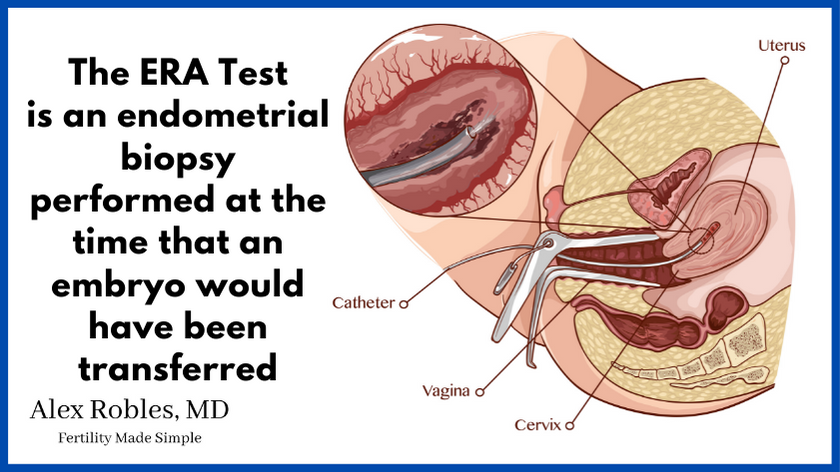
It is believed that there is a very small implantation window in which the endometrium can accept an embryo.
ERA attempts to determine when in your cycle this window is most optimal.
Unfortunately, this test is not yet proven technology.
Why does IVF fail In general?
There are many reasons why IVF can fail. Common causes include:
- Ovarian factor (due to a decrease in egg quality or egg quantity, often associated with increased maternal age)
- Male factor (poor sperm quality or quantity which can affect embryo growth and development)
- Embryonic factor (issues with the embryo itself)
- Endometrial factor (an inherent problem with your lining or uterine cavity that disrupts implantation)
- Tubal factor (dilated fallopian tubes aka hydrosalpinx can affect implantation)
- Laboratory quality control (the ability of the IVF laboratory to culture and handle embryos successfully)
As you can see, there is no one factor why IVF treatment fails in all cases.
Every couple has a slightly different situation, and your fertility specialist can give you an individual assessment of your prognosis.
In most cases, the most common reason for an unsuccessful cycle is diminished ovarian reserve from maternal aging.
How soon after failed IVF can I try again?
You can try again right away with your next cycle. You don’t necessarily need to wait a certain amount of time unless your doctor wants to do any additional testing or you need time to process your options.
Next steps after failed fertility treatment
When facing a failed treatment cycle, the best thing is to talk to your reproductive endocrinologist about determining the next steps.
Every couple and situation is different.
IVF failure does not necessarily mean the end of your fertility story. Many couples often need to undergo more than one IVF cycle and more than one embryo transfer.
With that said, it is essential to understand success rate statistics for couples with your demographics.
What are realistic success rates after failed IVF?
In general, each cycle’s IVF success rates (defined as having a live birth) tend to decrease over time.
However, the cumulative chance of having a live birth increases with the number of cycles you do.
This is true particularly true in cases where you are able to freeze embryos from more than one cycle.
The success rate of the second IVF cycle was about 25%; however, taken together, the cumulative live birth rate after two cycles was about 47%.
The third cycle had approximately a 23% chance of success, whereas three total cycles yielded a cumulative live birth rate of 58%.
The exciting thing is that the cumulative live birth rate actually continued increasing up to the 9th round of IVF!
It’s important to note that their research showed lower success rates for women >40 years of age.
For women between the ages of 40-42, the cumulative live birth after the first cycle was 12%, after two cycles 20%, and after three cycles ~25%.
In women older than 42, the cumulative live birth rate after two cycles was 7%, and after three cycles was 10%.
Other Related Questions
Are you more fertile after failed IVF?
You are not any more fertile after a failed cycle of IVF. Overall, pregnancy rates are roughly the same.
In addition, your fertility is not negatively impacted in any way from doing an IVF cycle.
Are there any signs that an embryo transfer did not work?
There are no signs that indicate whether an embryo transfer has worked or not. Your only way to know for sure is through the pregnancy test ~2 weeks after your transfer.
Is it possible to get an early period after a failed IVF cycle?
In general, periods tend to come as expected.
However, if you had a fresh embryo transfer and used Leuprolide as your trigger shot for the egg retrieval, it is possible to get a period a little earlier than expected.
Conclusion
It’s never easy to handle a failed IVF attempt.
Talk to your doctor about the results from your failed fertility treatment so that they can help you determine the next step that needs to be taken.
Try your best not to compare yourself with others who seem to be getting pregnant right away.
Remember that every person is different, and every pregnancy takes its own amount of time. Don’t give up!
Other Related Articles:
- Embryo Development: How Many Embryos Can You Expect To Make Per Cycle?
- Pre-implantation Genetic Screening: What Do The Results Actually Mean?
- What You Should & Should Not Do After A Frozen Embryo Transfer
Make An Appointment With Dr. Robles To Discuss Your Fertility Options Today!

Alex Robles, MD
Dr. Alex Robles is a Spanish-speaking Latino-American Reproductive Endocrinologist and Infertility specialist in New York City, and a board-certified OBGYN. He has a special interest in health, lifestyle, & nutrition. Make an appointment with Dr. Robles to discuss your fertility options today!
References:
- Zion Ben Rafael, Endometrial Receptivity Analysis (ERA) test: an unproven technology, Human Reproduction Open, Volume 2021, Issue 2, 2021, hoab010, https://doi.org/10.1093/hropen/hoab010
- Bhattacharya S, Maheshwari A, Mollison J. Factors associated with failed treatment: an analysis of 121,744 women embarking on their first IVF cycles. PLoS One. 2013;8(12):e82249. Published 2013 Dec 5. doi:10.1371/journal.pone.0082249
- Jacobs MB, Klonoff-Cohen H, Agarwal S, Kritz-Silverstein D, Lindsay S, Garzo VG. Predictors of treatment failure in young patients undergoing in vitro fertilization. J Assist Reprod Genet. 2016;33(8):1001-1007. doi:10.1007/s10815-016-0725-1
- Smith ADAC, Tilling K, Nelson SM, Lawlor DA. Live-Birth Rate Associated With Repeat In Vitro Fertilization Treatment Cycles. JAMA. 2015;314(24):2654-2662. doi:10.1001/jama.2015.17296
