Quick Answer
- Anti-Mullerian hormone, or AMH, is a hormone produced by the ovaries. It helps gauge ovarian reserve (the remaining number of eggs left in your ovaries.)
- A higher level indicates a greater number of eggs in reserve. As women age, AMH levels decline in a predictable pattern up until perimenopause.
- The best use of AMH testing is for determining IVF success. AMH impacts how well you’ll respond to fertility treatment.
- AMH does not tell you anything about the quality of the eggs. As such, a low level does not mean you are infertile.
What Does The AMH Test Measure?
Anti-müllerian hormone (AMH) provides a quantitative way of knowing how many eggs remain in your ovaries.
The higher the AMH level, the more eggs you have left in reserve. On the other hand, low levels of AMH indicate you have fewer eggs.
Fertility doctors can use this test to predict how your body will respond to ovarian stimulation. All things being equal, someone with higher AMH levels will respond better to fertility treatment.
AMH can also guide decisions on fertility preservation. A low level can help guide prompt family planning or advanced fertility treatments.

What Is A Normal Level?
A normal level of AMH is between 1.0 and 4.0 ng/mL. However, AMH levels vary considerably between women of similar ages.
Generally speaking, women in their late 20s have higher levels than women in their mid-30s. Those nearing menopause have lower levels.
An AMH under 1 ng/mL indicates a low ovarian reserve.
Always discuss your results with an experienced reproductive endocrinologist.
What Is A Good Level For IVF?
An average AMH level for a 35 year old is around 1.5 to 2 ng/mL. If you are 40, a level greater than 1 ng/mL is above average.
Conversely, if you are 30 or younger, a level greater than 2.5 ng/mL is average.
Who Should Consider Testing Their AMH?
AMH testing provides valuable information to several groups:
- Those undergoing fertility treatments like intrauterine insemination (IUI) or in vitro fertilization (IVF). AMH helps customize stimulation protocols.
- Individuals who are considering egg freezing for later family planning. It offers a baseline measure of your current reserve.
- Patients about to start cancer treatment endangering fertility. The level informs fertility preservation candidacy and urgency.
- If you think you have polycystic ovary syndrome (more on that later).
- Those with a family history of early menopause. An AMH blood sample may identify if you are at higher risk as well.
How To Prepare For The Test
The AMH test requires minimal preparation as it is a simple blood test.
You do not need any special dieting or lifestyle changes before the test. You also do not have to be fasting.
The other nice thing is that you can schedule it anytime in your menstrual cycle.
Also, you do not need to stop hormonal birth control or have an intrauterine device (IUD) removed.
When Should You Avoid Getting Your Levels Tested?
While AMH is valuable for many women, there are some situations where the results may not be accurate.
- If you’ve recently given birth or are breastfeeding, AMH will be lower than expected. It’s best to wait at least six months postpartum before you check the levels.
- If you have been using hormonal contraceptives for a while, your AMH level may be artificially lower than average. If your levels come back low, consider stopping the pills for one to two months before rechecking them.
- Prior surgery – Ovarian surgery like cyst removal can damage ovarian tissue and lower AMH. The effect depends on how much tissue is removed.
Other Factors Affecting AMH Levels
Your AMH level can fluctuate throughout your life for a variety of reasons. Here are some of the key factors that impact AMH:
- Age – AMH declines as you get older. An older woman will generally have a lower AMH than a younger woman. The decline accelerates after age 32 to 35.
- Overall health – Chronic conditions like obesity, diabetes, and untreated thyroid disorders can adversely affect ovarian reserve.
- Genetics – Some women are born with higher or lower AMH levels at baseline.
- Smoking – Cigarette smoking lowers AMH levels. Studies show that smoking can accelerate ovarian aging by two years.
- Cancer treatment – Chemotherapy and radiation therapy are toxic to ovaries and can rapidly diminish ovarian function.
Limitations of The Test
While AMH is the best marker of ovarian reserve, there are some important limitations.
First, AMH is an indirect measurement. It does not reveal the exact number of eggs left. Instead, it provides a rough marker of where you are relative to others your age.
Secondly, it only tests egg quantity. An AMH level does not tell you anything about the quality of the eggs.
As such, a normal AMH does not guarantee future fertility. Conversely, a low level does not mean you will have fertility issues.
However, higher levels of AMH correlate with better chances of successful IVF outcomes.
Given these limitations, you must interpret an AMH result with other clinical factors.
What To Do If You Have A Low Reserve
If you have a low AMH level, the first thing you should do is speak with a fertility specialist.
Your doctor can provide more context and help review your fertility potential.
They will also guide you with the best options for maximizing the likelihood of a future pregnancy.
If you are not interested in fertility, they can also counsel you on how to manage the decrease in ovarian function in the long term. Don’t do this alone!
Other Frequently Asked Questions
Can AMH Predict PCOS?
Polycystic ovarian syndrome (PCOS) is a hormonal disorder characterized by three things.
- Polycystic appearing ovaries: This is a misnomer – it should be “poly-follicular ovaries,” as these patients have many follicles, not cysts. A follicle contains an egg, whereas a cyst does not.
- High androgen levels: Androgens (male hormones) are produced in high amounts in women with PCOS, leading to symptoms such as acne or excess body hair growth.
- Irregular menstrual cycles: Women with PCOS often have irregular periods due to the abnormal hormone balance.
Since PCOS patients have a lot of ovarian follicles, by default, they should have a high AMH.
It’s true.
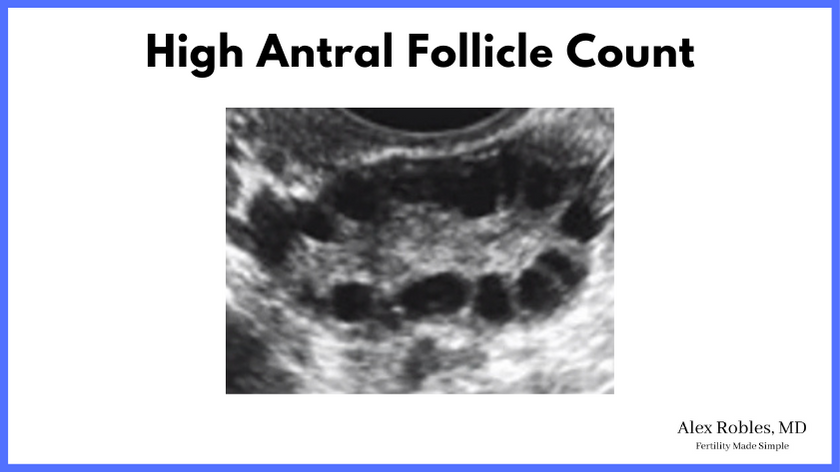
Women with PCOS tend to have high levels of AMH. However, AMH alone cannot diagnose the condition. An elevated AMH in the setting of irregular cycles may raise suspicion for the condition. However, it is not an official diagnostic criteria.
Keep in mind that a high AMH does not always indicate a problem. Some women without PCOS can have a high ovarian reserve. On the other hand, a normal AMH does not rule out PCOS.
Can It Predict Time To Menopause?
Since AMH reflects ovarian aging, very low levels signal you are nearing menopause.
However, AMH alone cannot predict when you will have your final period. Levels can bottom out years before the ovaries fully shut down.
Even peri-menopausal symptoms like hot flashes, insomnia, and vaginal dryness can occur years before menopause sets in.
Conclusion
The AMH test can provide valuable insight into your egg supply and how you will respond to ovarian stimulation.
However, no test result tells the whole story or predicts future fertility.
While AMH is a vital fertility marker, you must interpret it carefully. Age, health history, antral follicle count, and sperm health all matter.
Egg quality also matters a lot. Unfortunately, there is no way to determine egg quality before IVF treatment.
Make An Appointment With Dr. Robles To Discuss Your Fertility Options Today!

Alex Robles, MD
Dr. Alex Robles is a Spanish-speaking Latino-American Reproductive Endocrinologist and Infertility specialist in New York City, and a board-certified OBGYN. He has a special interest in health, lifestyle, & nutrition. Make an appointment with Dr. Robles to discuss your fertility options today!
