In this post, you are going to learn what the differences are between IUI and IVF.
Specifically, you’ll learn when and why you would go with one or the other.
Let’s get started.
What is IUI?
Intrauterine insemination (IUI) is a procedure where sperm is placed into your uterus using a thin, flexible tube around the time of ovulation.
The insemination can be done in a natural cycle (no medications) or after ovulation induction (with oral medications or injectable medications).
The advantage of an IUI over regular intercourse is that you bypass the cervix and place a high number of sperm closer to the fallopian tube, where it meets the egg before fertilization.
What is IVF?
In vitro fertilization (IVF) is a more invasive fertility treatment that involves
- daily injections to stimulate your ovaries to grow multiple eggs,
- removing the eggs from your ovaries under light sedation,
- fertilizing the eggs with sperm in the IVF lab,
- allowing the embryos to grow in an incubator,
- and then transferring the embryo(s) into your uterus.
Which one is better/more successful?
IUI success rates are typically around 10% per month, with an average of 2-3 cycles needed before pregnancy is achieved.
However, success rates largely depend on the age of the female partner and the diagnosis of both the male and the female couple.
Compiling the number from several studies, here are typical IUI success rates based on age: (study 1) (study 2) (study 3)
- <35 years of age: 10-14% per cycle
- 35-37 years of age: 9-10% per cycle
- 38-40 years of age: 7-8% per cycle
- 41+: 3-8% per cycle
IVF has much higher success rates, ranging from 30-50% per cycle in patients between 30-37 years of age.
After 38, success rates decline with a significant decrease after 41.
Here are the 2018 IVF success rates based on the CDC:
- <35 years of age: 52% per cycle
- 35-37 years of age: 38% per cycle
- 38-40 years of age: 23.5% per cycle
- 41-42 years of age: 11.2% per cycle
So here is a head-to-head comparison.
| Age | IUI Success Rates | IVF Success Rates |
|---|---|---|
| <35 | 10-14% | 52% |
| 35-37 | 9-10% | 38% |
| 38-40 | 7-8% | 24% |
| 41-42 | 3-8% | 11% |
Why would you do IUI instead of IVF?
While IUI does have a lower success rate than IVF, there are three reasons why you would choose IUI.
- Cost
- Preference
- Prognosis
Let’s go over each one by one:
Price
The most significant reason you would choose IUI over IVF is that it is significantly less expensive.
In addition, IUI cycles are more likely to have insurance coverage. Some insurance companies might require you to undergo 2-3 IUI cycles before approving an IVF treatment cycle.
A typical IUI cycle can cost you ~$500-2,000. In contrast, an IVF cycle can cost $15,000-$20,000 or more.
Preference
Many people opt for IUI over IVF because it is less invasive, involves less medication, has fewer blood tests and appointments.
Thankfully, neither IUI nor IVF is painful.
Also, you might prefer a more natural approach to conception, i.e., letting the sperm fertilize the egg inside your body.
Prognosis
Another benefit to IUI is that it can have respectable pregnancy rates in patients who are “good prognosis patients.”
In these cases, you can achieve a live birth without the need for more aggressive reproductive technology.
Should you try IUI before IVF?
It is reasonable to consider IUI before IVF treatment if you are:
- <40 years old
- Your fallopian tubes are open and are not blocked
- You are willing to wait at least 2-3 cycles before changing your treatment plan
- You are using donor sperm (and no other significant fertility issues)
- You have ovulatory infertility (such as PCOS)
- There is some form of sexual dysfunction in either partner
- The male partner has a healthy sperm sample

Who shouldn’t try IUI?
On the other hand, you should likely go right to IVF if you are:
- >40 years old
- Have a low ovarian reserve
- Have blocked fallopian tubes
- The male partner has severe male factor infertility (like low sperm count)
- Have failed multiple IUI cycles in the past
- You want multiple children and want to have them as quickly as possible
Other Advantages IVF has over IUI
IVF is not only more effective than IUI, but it is also more efficient and gives you more options.
For example, if you make multiple embryos, you can freeze any additional embryos for future use.
As a result, you can have more than one child years apart without needing to repeat a cycle. (This is advantageous since your chances of conceiving decrease with age).
Secondly, with a frozen embryo, you may schedule the timing of your transfer for when it is convenient for you.
Thirdly, you can also perform an embryo biopsy before transferring the embryo, allowing for genetic screening for chromosomal abnormalities.
Lastly, you can choose the gender of the embryo you want to transfer (assuming you made at least one embryo of each) and had genetic testing.
So, unlike IUI, IVF allows you to:
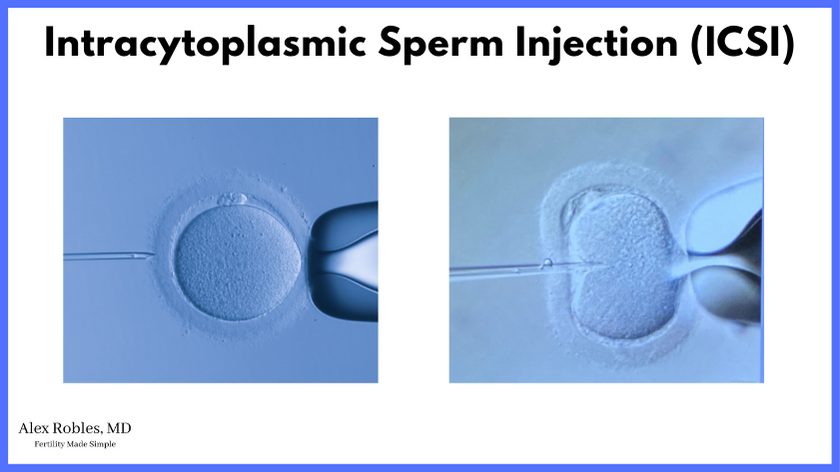
- Use ICSI, a procedure to select a single sperm to inseminate each egg (ideal for patients with severe male factor infertility)
- Freeze embryos to transfer at a date of your choosing
- Provides the possibility of more than one child if you make several embryos in one cycle
- Allows preimplantation genetic testing for chromosomal disorders
- Allows you to know the gender if you elect for genetic testing
Any fertility specialist will help you make a decision that is best for you and your specific case.
What medications are used for IUI?
Ovulation induction for IUI can be achieved with clomiphene citrate or letrozole. Both are oral medications that you only need to take for five days.
Rarely, injectable medications may also be used to stimulate your ovaries.
What medications are used for IVF?
IVF requires the use of injectable hormones. These include:
- FSH (Gonal-F, Follistim)
- LH (Menopur) *this medication is a combination of FSH and LH
- HCG or GnRH agonist (trigger shot)
Other related questions
What are the risks involved?
The most common risks associated with an IUI procedure include:
- Side effects from the medications (hot flashes, headaches, breast tenderness, dizziness)
- Small risk of infection from introducing a catheter into the uterus
- Small risk of ovarian hyperstimulation syndrome
- Higher risk of twins / higher-order gestation compared to IVF
The most common risks of an IVF cycle and procedure include:
- Side effects from the fertility medications (redness and pain at the injection site)
- Risks of egg retrieval procedure (bleeding, infection)
- Higher risk of ovarian hyperstimulation syndrome
- Higher risk of ectopic pregnancy compared to natural conception
Why is IUI more likely to result in multiple gestation than IVF?
IUI is more likely to result in twins or triplets because you cannot control how many follicles grow, and as a result, how many eggs are ovulated during a cycle.
If you have two or more follicles growing during an IUI cycle, you are at risk of getting pregnant with multiples.
With IVF, you can control the number of embryos that will be transferred back at a time.
In general, we will only transfer one embryo back into the uterus at a time.
What are the chances of twins in Either Approach?
- 1 Follicle: 4 %
- 2 Follicles: 12%
- 3 Follicles: 17%
- 4 Follicles: 20%
In other words, 4% of all the pregnancies achieved with 1 follicle were twin pregnancies, and 12% of all the pregnancies achieved with 2 follicles were twin pregnancies.
In contrast, the chance of a twin pregnancy after IVF depends on the number of embryos transferred. With a single embryo transfer, the likelihood of a twin pregnancy is about 1%. (This is due to monozygotic splitting: one embryo splitting into two, aka identical twins)
Is IUI worth the cost?
If you are a good candidate for IUI, it is well worth the cost if you can achieve a live birth without the need for in vitro fertilization.
However, if you are not an ideal candidate for IUI, it is more efficient to proceed directly with IVF.
Is IUI ever successful on the first try?
On average, you may have a ~10% chance of achieving a live birth on your first IUI cycle. The more IUI treatment cycles you do, the higher your cumulative chances of success.
Is it better to do IUI before or after ovulation?
The fertile window spans the five days before you ovulate, terminating on the day of ovulation.
It is still possible to get pregnant after ovulation provided the insemination happens on the same day.
An egg can only survive for 12-24 hours after it gets released, whereas sperm can survive in the female reproductive tract for ~3-5 days. As such, it is ideal to have intercourse or perform IUI before ovulation if possible.
Is an embryo transfer like an IUI?
Yes, the embryo transfer procedure is very similar to an IUI. Both use a tiny catheter that is introduced into your cervix to place the embryo or sperm into the uterus.
Unlike the IUI, the embryo transfer is done under ultrasound guidance to ensure that the embryo is placed in the correct location.
Conclusion
IUI can be an effective way to increase your chances of getting pregnant at a much lower cost than IVF.
With that said, IVF is more likely to result in a live birth, but it is more invasive and costly.
The most important things to consider are your personal preferences, financial situation, and the results you can expect based on your age/diagnosis.
Be sure to speak with a reproductive endocrinologist to learn the best option for you.
Related Articles:
- How Long Does IVF Take? The IVF Timeline
- How Long Does IUI Take? The IUI Timeline
- How Many Follicles Do You Need In IVF For Best Results?
- The Biological Clock In Women- Can It Be Stopped?
Make An Appointment With Dr. Robles To Discuss Your Fertility Options Today!

Alex Robles, MD
Dr. Alex Robles is a Spanish-speaking Latino-American Reproductive Endocrinologist and Infertility specialist in New York City, and a board-certified OBGYN. He has a special interest in health, lifestyle, & nutrition. Make an appointment with Dr. Robles to discuss your fertility options today!
References:
- Schorsch M, Gomez R, Hahn T, Hoelscher-Obermaier J, Seufert R, Skala C. Success Rate of Inseminations Dependent on Maternal Age? An Analysis of 4246 Insemination Cycles. Geburtshilfe Frauenheilkd. 2013;73(8):808-811. doi:10.1055/s-0033-1350615
- Haebe J, Martin J, Tekepety F, Tummon I, Shepherd K. Success of intrauterine insemination in women aged 40-42 years. Fertil Steril. 2002 Jul;78(1):29-33. doi: 10.1016/s0015-0282(02)03168-0. PMID: 12095486.
- Ganguly I, Singh A, Bhandari S, Agrawal P, Gupta N. Pregnancy Predictors after Intrauterine Insemination in Cases of Unexplained Infertility: A Prospective Study. Int J Reprod Med. 2016;2016:5817823. doi:10.1155/2016/5817823
- Smith ADAC, Tilling K, Nelson SM, Lawlor DA. Live-Birth Rate Associated With Repeat In Vitro Fertilization Treatment Cycles. JAMA. 2015;314(24):2654-2662. doi:10.1001/jama.2015.17296
- Evans MB, Stentz NC, Richter KS, Schexnayder B, Connell M, Healy MW, Devine K, Widra E, Stillman R, DeCherney AH, Hill MJ. Mature Follicle Count and Multiple Gestation Risk Based on Patient Age in Intrauterine Insemination Cycles With Ovarian Stimulation. Obstet Gynecol. 2020 May;135(5):1005-1014. doi: 10.1097/AOG.0000000000003795. PMID: 32282611; PMCID: PMC7183886.
