Progesterone injections are a critical part of the in vitro fertilization process.
Without progesterone, your body would not be able to maintain a pregnancy.
In this post, you will learn:
- What progesterone shots do
- Side effects you might experience from the injections
- Tips for where to inject and how to do it
Let’s get started.
What are progesterone shots for in IVF?
Progesterone shots help your body prepare for embryo implantation and sustain the growth of an early pregnancy.
Progesterone is a hormone secreted by the corpus luteum. This structure forms in your ovary ONLY AFTER you ovulate.
As such, progesterone supplementation is necessary if you are doing an embryo transfer cycle in which you do not ovulate. This is the case if you choose to do a medicated frozen embryo transfer (FET) cycle rather than a natural FET cycle.
Without ovulation (and hence progesterone), an embryo wouldn’t be able to attach to the lining of the uterus and continue growing after implantation.
Do all IVF patients take progesterone?
In general, only patients who undergo an IVF cycle, freeze their embryos and subsequently undergo a frozen embryo transfer need to take progesterone.
- If you undergo a medicated frozen transfer cycle, you will need to take progesterone injections (as you do not ovulate in this cycle)
- If you undergo a natural frozen embryo transfer, your doctor may have you take vaginal progesterone suppositories, which are less potent than the injections
- If you undergo a fresh embryo transfer (a transfer in the same cycle as the egg retrieval), your doctor may have you take a vaginal suppository
In both the natural cycle and a fresh embryo transfer, you “ovulate”, and thus, produce natural progesterone. As a result, you don’t need an intramuscular progesterone injection.
Do IVF progesterone shots hurt?
Unfortunately, progesterone injections hurt more than the standard IVF stimulation medications.
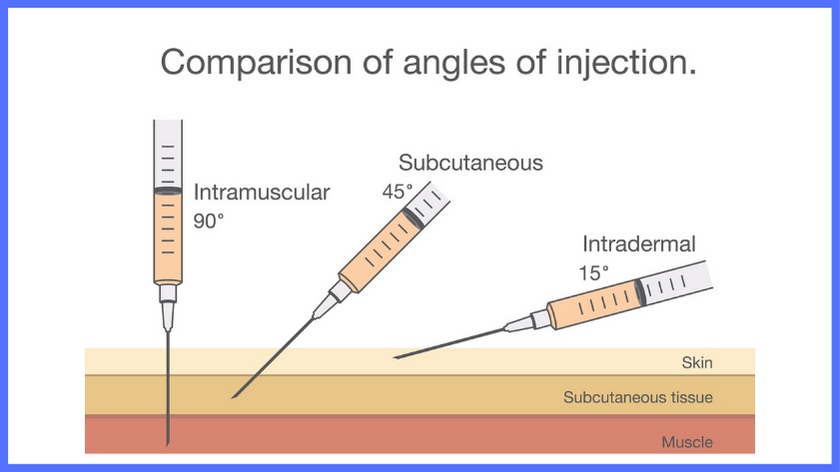
Progesterone is an intramuscular injection, meaning that the needle is bigger, and injected deeper than subcutaneous injections.
As a result, it can be more painful than the other IVF medications.
What are the side effects of progesterone injections?
The most common side effects of progesterone injections are related to your injection site.
These side effects include:
- Pain and discomfort around the injection site
- Swelling at the injection site
- Redness at the injection site
Rarely, some patients will have an allergic reaction to the oil in the progesterone formulation.
If you develop an allergic reaction, your doctor can have the pharmacy change the oil that the progesterone is made in (usually from sesame oil to olive oil).
How quickly do progesterone injections work?
Progesterone injections work fairly quickly, usually reaching peak plasma concentration in about 8 hours and lasting up to 24 hours.
As such, the injections are administered daily (every 24 hours).
In what location should you administer your progesterone shots?
The progesterone injection is intramuscular, meaning it needs to be injected in a location with a large muscle group.
The most common area used is the upper outer quadrant of the buttock.
Another location is the outer side of the upper thigh, the vastus lateralis muscle.
Your preference determines the choice of the injection site. You may find it more comfortable to use one location over the other.
What should you do if you have pain with the progesterone injections?
There are two strategies for dealing with pain from progesterone injections.
The first is to use an ice pack on the injection site before and right after the injection. This often reduces the local inflammation, which sometimes helps with decreasing pain and discomfort.
The second strategy is to massage the area around the injection site after the cold pack. This enhances local blood flow and may also reduce some of the pain. A heating pad can also have the same effect.
If none of this helps, you can also apply a topical numbing cream to the injection site before cleaning it with alcohol.
Other tips for administering your progesterone shots
Rotate the sites
Another great tip for reducing discomfort from the injection is to rotate your injection sites (meaning you switch locations each time).
Most patients find it easy to inject in the right gluteal muscle one day, then the left glute the next day.
This will help avoid inflammation build-up in one area.
Get some help
Another option is to recruit someone to help you with your injections.
For example, you can have your partner or someone you trust to administer the injection. This way, you can focus on relaxing instead of being anxious about the pain while giving yourself an injection.
Let the alcohol dry
Before you administer the injection, make sure you clean the site with alcohol. However, do not proceed with the injection right away.
Let the alcohol dry first.
This may reduce some of the stinging that is associated with the shot.
Talk to your doctor about this study
A new study of over 1000 medicated FET cycles published in 2021 compared the use of:
- vaginal progesterone to
- intramuscular (IM) progesterone to
- alternating vaginal and intramuscular progesterone
They found no significant difference in live birth rates between the group that used IM progesterone alone and the group that alternated vaginal and IM progesterone.
Speak with your doctor to see if you are a candidate for this protocol so that you can use fewer injections and potentially have fewer side effects.
Another recent study also looked at the use of a vaginal gel and saw promising results.
How to give progesterone injections to yourself
What if you don’t have someone to help you with the injection? Here is a step-by-step process of how you can self-administer a progesterone injection.
- Wash your hands with soap and water, and gather all of your items
- Clean the injection site with alcohol and let the alcohol dry
- It is essential to use a new alcohol swab each time you clean your injection site. This will help avoid any infection and also reduce the pain from the injection
- Uncap the progesterone medication and clean the top of the vial with an alcohol swab
- After cleaning with alcohol, uncap the needle and pull back on the plunger of the syringe to get air in the syringe
- You will then insert the needle into the vial and push the air in, which will help you pull out the medication
- Flip the vial upside down so that the needle is pointing upward, and pull back on the plunger to pull out the required amount of medication
- Make sure that the tip of the needle is under the fluid at all times
- Remove the needle from the vial and make sure that there are no air bubbles
- Holding the needle like a dart, insert the needle at a 90-degree angle to your skin and into the muscle
- Pull back on the syringe to look for blood. If there is blood, the tip of the needle is in a blood vessel
- If this is the case, remove the needle, recap it and throw it away in a proper container. Unfortunately, you have to start the process over
- If you don’t see blood, inject the medication slowly, taking about 10 seconds for the injection
- After injecting all of the progesterone, remove the needle, recap it, and throw it away in the proper container
- Apply pressure to the injection site and place a bandaid if desired
When can I stop taking progesterone? How long do you need to take it?
Progesterone injections are usually given daily for up to 10 weeks of pregnancy (about 8 weeks post embryo transfer).
At ~8 weeks of pregnancy, the placenta takes over the function of progesterone production.
In theory, progesterone shots can stop at that time. Still, most fertility specialists prefer to overlap additional progesterone with your endogenous progesterone.
Do not discontinue your progesterone support until your doctor has confirmed that you no longer need it!
Will I miscarry if I stop taking progesterone?
If you stop your progesterone too early, you may be at risk of having a miscarriage. This is particularly true if you had a medicated frozen embryo transfer.
Always be sure to speak with your doctor before you stop taking your daily injections of progesterone.
Is it safe to stop progesterone at 10 weeks?
By 10 weeks of pregnancy, the placenta has taken over the job of progesterone production.
This is known as the luteal placental shift.
Most fertility specialists will have you stop your progesterone supplementation at this time, especially if your progesterone levels are adequate on blood tests.
I go over this in more detail in my post on when to stop estrogen and progesterone.
Conclusion
Progesterone in oil injections are necessary for patients undergoing fertility treatment with a medicated FET cycle.
The progesterone shot may be given daily for up to 10 weeks of pregnancy (which is about 8 weeks post embryo transfer).
If you underwent a natural frozen embryo transfer cycle, your doctor will likely recommend a different form of progesterone for luteal support.
As always, it is essential to follow the instructions from your fertility specialist regarding how long this treatment should last.
Related Articles:
- The Frozen Embryo Transfer Timeline: How Long Does It Take
- Embryo Tranfer Precautions: What You Should & Shouldn’t Do
- When Can You Stop Estrogen After IVF?
Make An Appointment With Dr. Robles To Discuss Your Fertility Options Today!

Alex Robles, MD
Dr. Alex Robles is a Spanish-speaking Latino-American Reproductive Endocrinologist and Infertility specialist in New York City, and a board-certified OBGYN. He has a special interest in health, lifestyle, & nutrition. Make an appointment with Dr. Robles to discuss your fertility options today!
References:
- Csapo AI, Pulkkinen MO, Ruttner B, Sauvage JP, Wiest WG. The significance of the human corpus luteum in pregnancy maintenance. I. Preliminary studies. Am J Obstet Gynecol. 1972 Apr 15;112(8):1061-7. doi: 10.1016/0002-9378(72)90181-0. PMID: 5017636.
- Devine K, Richter KS, Widra EA, McKeeby JL. Vitrified blastocyst transfer cycles with the use of only vaginal progesterone replacement with Endometrin have inferior ongoing pregnancy rates: results from the planned interim analysis of a three-arm randomized controlled noninferiority trial. Fertil Steril. 2018 Feb;109(2):266-275. doi: 10.1016/j.fertnstert.2017.11.004. Epub 2018 Jan 17. PMID: 29338855.
- Devine K, Richter KS, Jahandideh S, Widra EA, McKeeby JL. Intramuscular progesterone optimizes live birth from programmed frozen embryo transfer: a randomized clinical trial. Fertil Steril. 2021 Sep;116(3):633-643. doi: 10.1016/j.fertnstert.2021.04.013. Epub 2021 May 13. PMID: 33992421.
- Bakkensen JB, Racowsky C, Thomas AM, Lanes A, Hornstein MD. Intramuscular progesterone versus 8% Crinone vaginal gel for luteal phase support following blastocyst cryopreserved single embryo transfer: a retrospective cohort study. Fertil Res Pract. 2020;6:10. Published 2020 Jul 1. doi:10.1186/s40738-020-00079-y
