In this article, you will learn:
- what a trigger shot is used for in IVF
- when is the best time to take it
- what happens if you miss the timing
- and much more.
Let’s get started.

What is a trigger shot?
A trigger shot is a medication given during an intrauterine insemination (IUI) or an in vitro fertilization (IVF) cycle to induce ovulation.
In other words, it is given to know the exact timing in which the follicles in your ovary will rupture and release the eggs they contain.
That way, we can plan to perform the egg retrieval (or IUI) just before you release the eggs.
When is the trigger shot given in IVF?
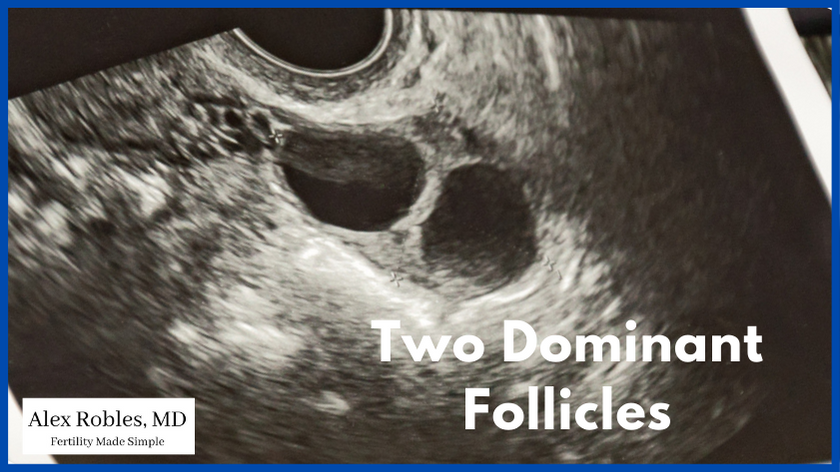
In IVF, the trigger shot is administered on the day that your follicles have grown to an optimal size. This typically means that you have two or more follicles that are 18 mm in size or greater.
In most cases, the shot is administered on days 8-12 of an IVF cycle, depending on how quickly your follicles grow.
Does a trigger shot guarantee ovulation?
A trigger shot essentially guarantees ovulation, but nothing is 100%.
We administer a trigger for two reasons:
- It induces the egg(s) to mature: (only mature eggs can be successfully fertilized and implanted).
- It helps to give us more control over exactly when your egg(s) will be ovulated
However, not every egg will mature after a trigger shot, and some women can ovulate before the retrieval even occurs.
Our goal is to give the eggs enough time to mature but retrieve them before they are released.
What happens if you take the trigger shot late?
If you take your trigger injection late, we may need to change the timing of your egg retrieval.
The goal is to have the retrieval done ~36 hours after the injection. If you are late by 30 minutes or so, it probably won’t make a significant difference. There is approximately a 1 hour window of wiggle room.
If you are late by more than an hour, that would almost certainly change the timing of your retrieval.
What happens if I miss the trigger shot or I take it the next day?
If you miss your trigger shot or take it a day late, then you are at risk of ovulating prematurely.
This is especially true if you had a premature luteinizing hormone LH surge on your hormone testing.
In this case, call your fertility doctor’s office immediately.
Most of the time, taking an extra dose of the GnRH antagonist medication could potentially prevent premature ovulation.
What medication is used for a trigger shot in IVF?
There are two types of trigger injections: hCG and Leuprolide (aka Lupron).
The standard trigger shot medication is human chorionic gonadotropin (hCG).
Yes, this is the pregnancy hormone.
We use hCG in an IVF cycle because it has the same chemical structure as luteinizing hormone.
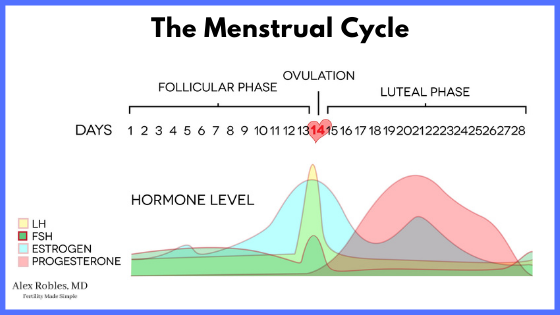
In other words, the trigger shot mimics the luteinizing hormone (LH) surge that occurs ~36 hours before ovulation in a natural menstrual cycle. Therefore, your body interprets the trigger shot as an LH surge.
Leuprolide works differently.
The GnRH agonist trigger shot works by inducing your pituitary gland to release a massive amount of FSH and LH.
You will still have an “LH surge,” but it comes from your own body, rather than externally, like in the case of the hCG shot.
Is the trigger shot painful?
Trigger shots are not painful. They are typically injected subcutaneously (even though some boxes say intramuscular injection), which can cause minor discomfort at the injection site.
How do you feel after an IVF trigger shot?
You probably won’t feel any different after your trigger shot. With that said, many patients already feel bloated by the time they take the injection.
How do I know if my trigger shot worked?
One easy way to know that your trigger shot worked is to check a urine pregnancy test ~12 hours after an hCG injection.
If the test is positive, then we know that it took effect. Many fertility clinics will have you come in the day after your trigger shot for a blood test to check your hCG levels.
Similarly, you can check an ovulation predictor kit ~12 hours after a Lupron trigger to confirm that your LH levels are elevated.
What are the side effects of an hCG trigger shot?
The side effects of hCG are similar to the other fertility medications you have already been taking.
Common adverse effects you may experience include:
- Headache
- Fatigue
- Abdominal bloating
- Pain or redness at the injection site
In addition, hCG carries a higher risk of ovarian hyperstimulation syndrome (OHSS). Thankfully, moderate and severe OHSS is quite rare, and we have many different ways to manage it.
What are the names of different trigger shots?
HCG trigger shots have many different names. The most common brand names in America are:
- Pregnyl
- Novarel
- Ovidrel
- or just HCG
The GnRH agonist trigger shot is called:
- Leuprolide or Lupron.
Other Related Questions
Why do you get 2 trigger shots IVF?
More and more research is coming out that patients who use both trigger shots, hCG and Lupron, have increased:
– number of embryos produced, and
– clinical pregnancy rates compared to hCG alone.
Physiologically, you are getting both an internal and external source of LH for a more robust surge.
Secondly, using Lupron allows you to decrease the dose of hCG needed to induce final egg maturation. A lower dose of hCG can significantly reduce your risk of OHSS.
Many clinics are starting to use this dual-trigger option exclusively to optimize success rates.
Is a trigger shot necessary for IVF?
Your entire IVF treatment cycle depends on the trigger shot.
Without a trigger shot, we wouldn’t be able to predict when you are going to ovulate!
It’s the only way to control when your egg retrieval procedure will be, which is crucial to optimize success.
Do eggs grow after the trigger shot?
Your follicles will not continue to grow after a trigger shot. The surge that occurs as a result of the trigger is what begins the process of oocyte maturation, which is the next phase after follicle growth.
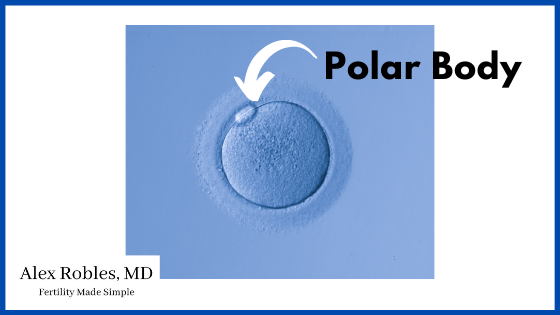
Mature eggs have a polar body.
What should I eat after trigger shot IVF?
After your trigger medication, you should stay well hydrated with electrolyte-rich fluids. We often recommend natural coconut water.
You should also try to eat a well-balanced diet just for overall health.
Can you ovulate 12 hours after the trigger shot?
It is unlikely that you will ovulate 12 hours after a trigger shot unless your body is already experiencing a premature LH surge.
We will be able to detect this on your blood work.
Unfortunately, some patients with a diminished ovarian reserve are at risk of early ovulation, but this usually occurs around 24-34 hours after the trigger.
Is a trigger shot necessary for an IUI cycle?
The trigger injection is beneficial in an IUI cycle because it lets us know the specific time for the insemination.
However, an IUI cycle is not dependent on the trigger to be successful.
- You will eventually surge on your own no matter what
- The timing of the IUI isn’t as critical as an egg retrieval, i.e, sperm can survive in the female reproductive tract for several days.
The key is to do the intrauterine insemination or have timed intercourse before you ovulate!
Final Words
The trigger shot is an integral part of the IVF process. It helps to ensure that your body prepares your ovarian follicles for ovulation and allows us to schedule your egg retrieval appropriately.
Please make sure that you have this vital medication as the entire IVF cycle depends on it!
Other Related Articles:
- The IVF Timeline: How Long Does An Ovarian Stimulation Cycle Take?
- 9 Common Side Effects of Fertility Drugs & Injectable Medications
- The Egg Retrieval Day: What To Expect & How To Prepare For It
Make An Appointment With Dr. Robles To Discuss Your Fertility Options Today!

Alex Robles, MD
Dr. Alex Robles is a Spanish-speaking Latino-American Reproductive Endocrinologist and Infertility specialist in New York City, and a board-certified OBGYN. He has a special interest in health, lifestyle, & nutrition. Make an appointment with Dr. Robles to discuss your fertility options today!
References:
- Haas J, Bassil R, Samara N, Zilberberg E, Mehta C, Orvieto R, Casper RF. GnRH agonist and hCG (dual trigger) versus hCG trigger for final follicular maturation: a double-blinded, randomized controlled study. Hum Reprod. 2020 Jul 1;35(7):1648-1654. doi: 10.1093/humrep/deaa107. PMID: 32563188.
- Şükür YE, Ulubaşoğlu H, İlhan FC, Berker B, Sönmezer M, Atabekoğlu CS, Aytaç R, Özmen B. Dual trigger in normally-responding assisted reproductive technology patients increases the number of top-quality embryos. Clin Exp Reprod Med. 2020 Dec;47(4):300-305. doi: 10.5653/cerm.2020.03804. Epub 2020 Oct 28. PMID: 33113599; PMCID: PMC7711097.
- Chern CU, Li JY, Tsui KH, Wang PH, Wen ZH, Lin LT. Dual-trigger improves the outcomes of in vitro fertilization cycles in older patients with diminished ovarian reserve: A retrospective cohort study. PLoS One. 2020 Jul 6;15(7):e0235707. doi: 10.1371/journal.pone.0235707. PMID: 32628729; PMCID: PMC7337315.
- El Tokhy O, Kopeika J, El-Toukhy T. An update on the prevention of ovarian hyperstimulation syndrome. Womens Health (Lond). 2016;12(5):496-503. doi:10.1177/1745505716664743

why do you think we should take only IM progesterone and not suppository only?
It depends on the type of embryo transfer cycle you are doing- in some situations the suppository can be effective. I go over this in more detail here: https://alexroblesmd.com/progesterone-injections-ivf/