In this post, you’re going to learn:
- What a follicle is,
- How many follicles is considered a “good” number, and
- What facilitates follicular growth during in vitro fertilization cycles.
Let’s get started.
What is a follicle?
Follicles are small, fluid-filled sacs that form on your ovaries. These little sacs contain developing eggs.
You can begin to see small follicles forming at the beginning of your menstrual cycle, and they grow over time as your cycle progresses.
Ultimately, only one follicle will grow each month while the rest will degenerate. The single lead follicle will eventually rupture, releasing a mature egg in a process known as ovulation.
In an IVF cycle, the goal is to grow MULTIPLE follicles at once, something that does not occur in a natural cycle.
What does the number of follicles mean?
We use the antral follicle count (the number of follicles we see on transvaginal ultrasound at the beginning of your menstrual cycle) for two things:
- It helps to determine your ovarian reserve, and
- it helps to predict how your body will respond to ovarian stimulation.
In other words, the more follicles we see, the more eggs you have remaining in your ovaries, and the more likely you will respond to the fertility medications.
Blood tests can also help measure your reserve, specifically the AMH, or anti-mullerian hormone.
How many are normal for IVF?
In general, we like to see around 6-8 follicles per ovary, but there is a lot of variety between patients, and this number naturally decreases with age.
With that said, it is important to note that quantity isn’t the only factor.
Egg quality and sperm quality also play a big role as well. Unfortunately, quality isn’t something that can be tested beforehand, while quantity is very easy to measure.
Be sure to speak with your doctor to discuss expectations regarding your follicle count and AMH level.
What helps Them grow?
Follicles grow in response to the hormone follicle stimulating hormone (aka FSH). This is a hormone released from the pituitary gland, and its job is to recruit the development of a dominant follicle for ovulation.
That is why we prescribe high-dose injections of FSH for ovarian stimulation. The goal is to grow as many ovarian follicles as safely possible.
However, there are diminishing returns.
More FSH isn’t always better.
Do all follicles grow in response to stimulation?
Unfortunately, not every one of your follicles will grow during an IVF stimulation. There is no way to predict which follicles will grow and which ones will regress.
Larger follicles are always more likely to grow compared to smaller ones.
How many mm do follicles grow each day?
In general, most follicles will grow about 1-2 mm per day, but this can vary among patients.
Our goal is to grow ~2-3 follicles to ~18 mm in size before doing an oocyte retrieval. The closer the follicle is to 18 mm in size, the more likely the egg obtained will be mature.
It is possible that a 13-17 mm follicle will yield a mature egg, but it is less likely.
Here is a typical growth chart of what you might expect to see.
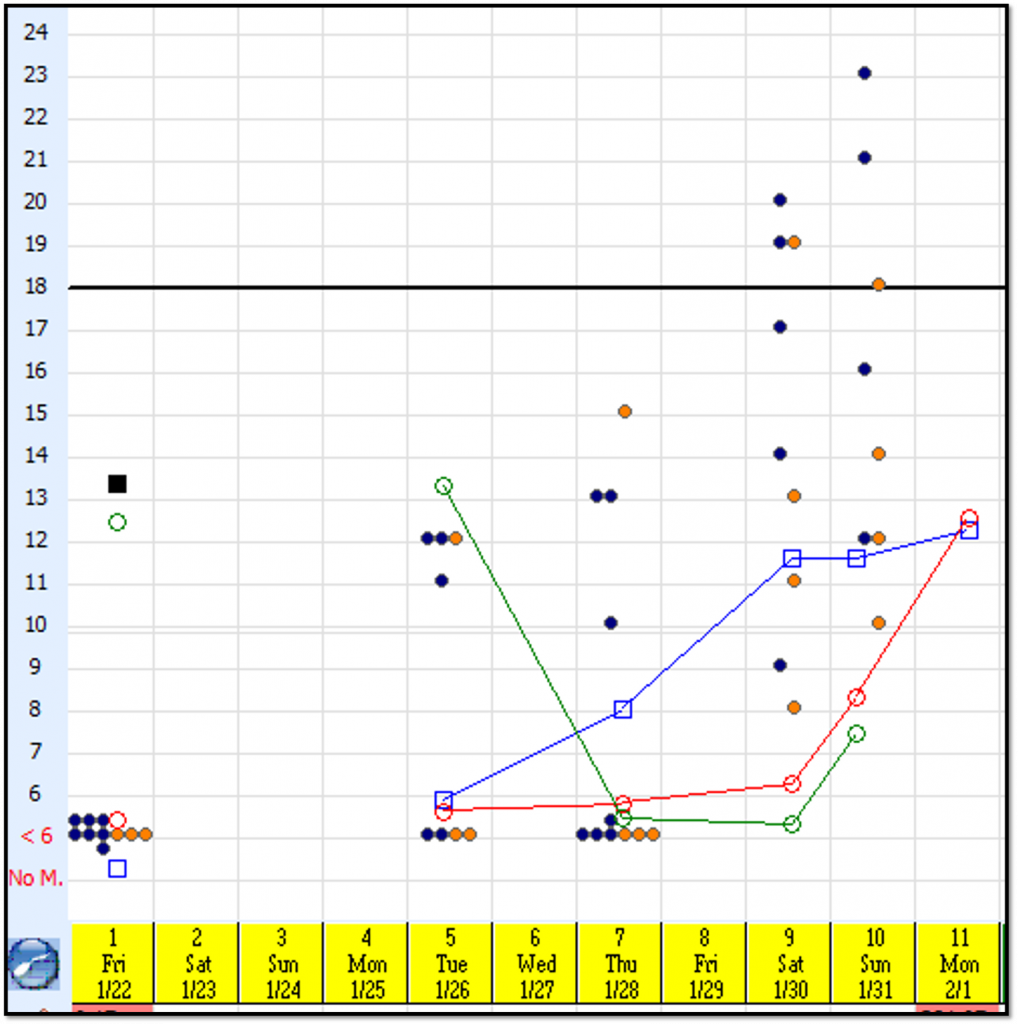
- Blue dots represent the number of follicles in the right ovary.
- Orange dots represent the number of follicles in the left ovary.
- The y axis represents the size of follicles in mm.
- The x axis represents the number of days since the stimulation has started.
- As you can see, on Day 1, there were 10 follicles less than 6 mm in size.
- By Day 5, three follicles reached 12 mm in size, and one 11 mm in size.
- By Day 9, three follicles have surpassed 18 mm in size.
Are _ # of follicles enough for IVF?
Many women wonder if 3, 4, 5, 6, 7, etc follicles are enough to have success with IVF.
This question is impossible to answer until we see:
- how many eggs are retrieved during your procedure
- how many of those eggs fully matured
- how many of the eggs fertilize
- how many of those fertilized eggs will grow and develop to the blastocyst stage
Some women will have a 30% conversion rate of the number of eggs retrieved to the number of blastocysts formed.
Some can have more, and some can have less.
Blastocysts don’t guarantee success either. You can expect a ~50% success rate (aka having a live birth) per embryo transfer of a good quality blastocyst.
So while having more follicles is generally better, it is not the only factor.
What is the average number of eggs retrieved in IVF?
On average, patients between 35-38 years of age will have approximately 10-12 eggs retrieved following an IVF treatment cycle.
This number can vary widely based on age and ovarian reserve. But in general, you can expect fewer eggs with increasing age.
Here are some rough approximations you could expect from databases of prior IVF patients based on age.
- <35 years old: ~15+ eggs
- 35-37 years old: ~12-15 eggs
- 38-40 years old: ~10-12 eggs
- 41-42 years old: ~4-8 eggs
- 43 and over: ~0-5 eggs
Keep in mind, these are averages. Your results may vary.
How can I increase my number of follicles?
Unfortunately, there is no way to increase the number of follicles you have. There will be cycle to cycle variability in the number of follicles you will have each month, but the number trends down with time.
We do know that smoking and other harmful lifestyle habits can worsen or expedite your rate of follicular loss.
Other Related Questions
How many eggs are in a follicle?
There can only be one egg per follicle.
However, it is possible to have an empty follicle with no egg. During a retrieval, all reasonably sized follicles (>10 mm in size) will be aspirated if it can be done safely.
But in general, up to 20% of follicles can be empty despite being the appropriate size.
What is a mature follicle- is that different from mature eggs?
There technically isn’t such a thing as mature follicles. Only the oocyte can be mature or immature.
With that said, the larger the follicular size, the more likely the egg will be mature.
What follicle size is ideal?
Ideally, a follicle should be between 16-22 mm in size. This will give it the best chance of yielding a mature oocyte.
Once 2-3 follicles have reached this size, we will administer a trigger shot to induce oocyte maturation.
It is possible to retrieve mature eggs from follicles smaller than 16 mm, but it is less likely.
This is the purpose of your morning ultrasound scans. To measure the size and growth of your follicles.
What size is too big?
There is no cut-off for how big a follicle can get, but in general, we do not like to see the size of the follicle surpassing 24-25 mm.
Large follicles are at risk of yielding post-mature eggs. This is a theoretical condition where the eggs are noted to mature but do not fertilize as expected (aka decreased fertilization rates).
There is also a risk of a large follicle rupturing and ovulating the egg it contains.
How many are too many?
There is no set number of follicles that are considered too many. Women with polycystic ovarian syndrome (PCOS) can often have 30 or more growing follicles.
The problem with a large number of follicles is that a high percentage of them can yield immature eggs.
In addition, very high follicle counts can increase your risk of developing ovarian hyperstimulation syndrome, or OHSS for short. This is a self-limiting condition that can cause significant discomfort and may require hospitalization in severe cases.
Conclusion
Follicle tracking is a very important factor that helps us determine how your body is responding to the IVF stimulation.
While the quantity of follicles is important, the quality of your eggs also plays an important role in terms of success rates.
Be sure to consult with a fertility specialist to learn what you can expect your ovarian response to be to fertility treatment!
Related Articles
- Immature Eggs: What Are They & What Can You Do About Them?
- Is IVF Painful? Here’s What To Expect
- How Many Blastocysts Can You Expect To Get From An IVF Cycle
Make An Appointment With Dr. Robles To Discuss Your Fertility Options Today!

Alex Robles, MD
Dr. Alex Robles is a Spanish-speaking Latino-American Reproductive Endocrinologist and Infertility specialist in New York City, and a board-certified OBGYN. He has a special interest in health, lifestyle, & nutrition. Make an appointment with Dr. Robles to discuss your fertility options today!
